Reliable Medical Billing & Coding Services
We hav e a 99.9% claim acceptance rate.
ClearCodeBilling provides end-to-end medical billing, coding, and revenue cycle management services for healthcare providers across the United States. We help practices increase revenue, reduce claim denials, and get paid faster while staying fully HIPAA compliant.

1200+ Providers Served
100+ Medical Specialties
500+ Certified Coders & Billers
50 States Served
Our Client Base
ClearCodeBilling provides comprehensive medical billing and revenue cycle management services to a diverse range of healthcare providers. We work closely with organizations of all sizes from independent practices handling daily billing challenges to large healthcare facilities managing high-volume operations.Our focus is on delivering customized billing solutions that improve cash flow, reduce denials, and increase overall operational efficiency.
Health
Care
Hospitals
Services
Emergency
Rooms
Mental
Health
Urgent
Care
Therapy
Services
Cardiology
intervention
Behavioral
Health
Home
Health
Radiology & Pain Mgmt
Pediatric
Care
Other
Specialties
Why Choose ClearCodeBilling as Your Medical Billing Partner
ClearCodeBilling provides reliable medical billing and revenue cycle management services designed to help healthcare providers improve collections and reduce administrative stress. Our certified billing and coding professionals ensure accurate claim submission, fewer denials, and faster reimbursements.
We focus on transparency, compliance, and personalized support. With detailed reporting and dedicated account management, ClearCodeBilling becomes a trusted billing partner—allowing you to concentrate on patient care while we optimize your revenue cycle.
Medical Billing Services & Solutions That Streamline Your Revenue and Improve Your Cashflow
Out of Network Negotiation
ClearCodeBilling specializes in out-of-network negotiation services to help healthcare providers maximize reimbursements. Our experienced team works directly with payers and pricing vendors to secure fair payments while reducing write-offs and revenue loss.
Credentialing & Contracting
We manage complete provider credentialing and payer contracting to ensure timely approvals and optimal reimbursement rates. Our streamlined process minimizes delays, prevents enrollment issues, and keeps your practice fully compliant with payer requirements.
Benefits of Choosing Our Medical Billing Services
ClearCodeBilling helps healthcare providers improve financial performance by reducing billing errors, accelerating reimbursements, and increasing overall revenue. Our structured billing workflows and certified experts ensure accuracy, compliance, and efficiency at every stage of the revenue cycle.
By outsourcing your medical billing to ClearCodeBilling, you gain dedicated support, transparent reporting, and scalable solutions tailored to your practice.

Focus on Patient Care
Reduced Admin Duties
Enhanced Cash Flow
Reduced Billing Errors
Patient Satisfaction
Secured Patient Data
Billing Compliance
Process Claims Faster
Is Your Practice Leaving Money
on the Table?
Many healthcare practices lose revenue due to coding errors, claim denials, underpayments, and inefficient billing processes. ClearCodeBilling identifies hidden revenue gaps and helps recover lost income through detailed audits and proactive revenue cycle management.
Our Medical Billing Process
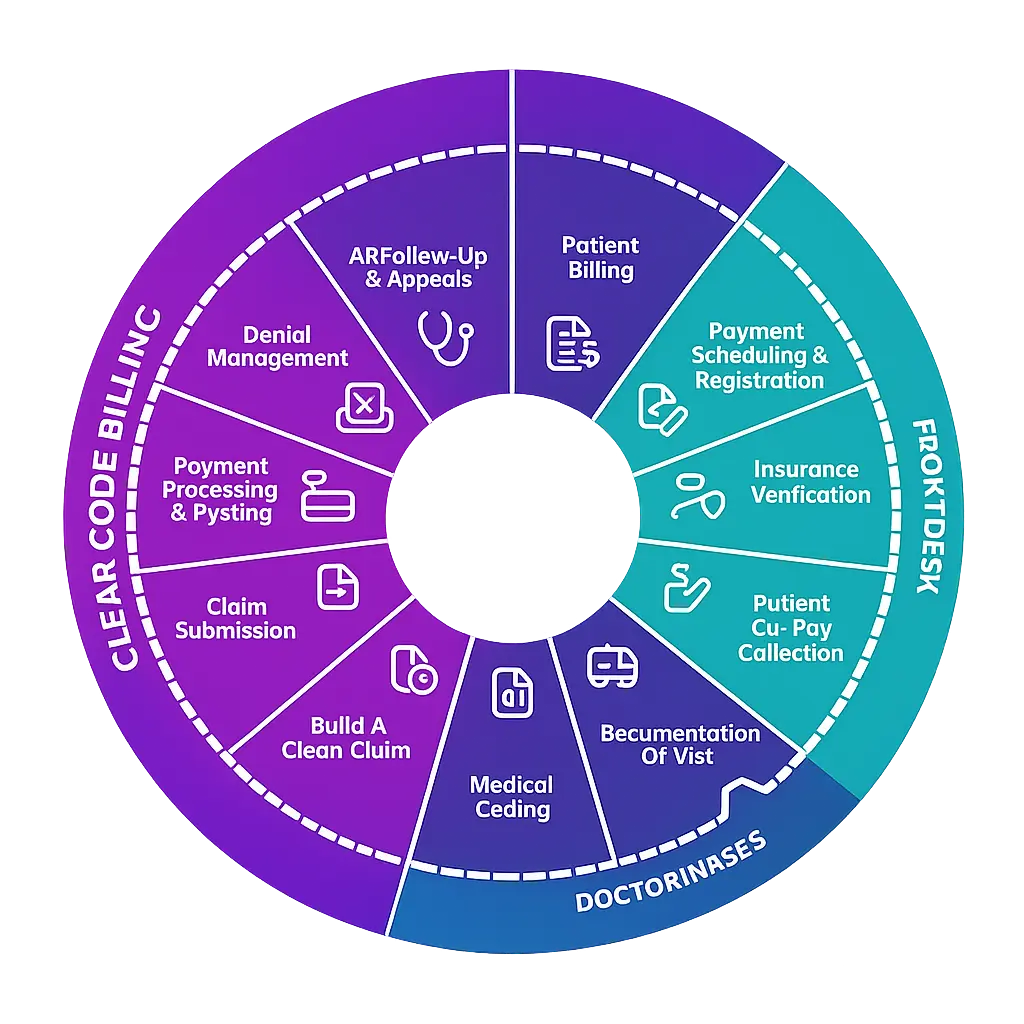
Provider Enrollment & Credentialing
We complete payer enrollment and credentialing to ensure providers are approved and reimbursed without delays.
Patient Registration & Insurance Verification
Insurance eligibility, benefits, and authorizations are verified upfront to prevent claim rejections.
Accurate Medical Coding
Certified coders assign precise ICD-10, CPT, and HCPCS codes to ensure compliance and maximum reimbursement.
Charge Entry & Claim Scrubbing
Claims are reviewed and scrubbed before submission to reduce errors and speed up processing.
Payment Posting & Reconciliation
Payments, ERAs, and EOBs are posted accurately, with discrepancies identified quickly.
Denial Management & Appeals
Denied and underpaid claims are analyzed and appealed aggressively to recover lost revenue.
Accounts Receivable Follow-Up
Dedicated AR specialists follow up consistently to reduce aging and improve cash flow.
Patient Billing & Support
Clear patient statements and responsive support enhance patient satisfaction and collections.
Reporting & RCM Insights
Transparent reporting and performance insights help practices monitor revenue and optimize operations.
